Articles & Resources
Hip Assessment by Logan Schwartz
Posted by Boston Sports Medicine and Performance Group on Nov 28, 2010 3:30:00 PM
Topics: Guest Author, Health & Wellness
Priciples Of The Hip by Logan Schwartz
Posted by Boston Sports Medicine and Performance Group on Nov 21, 2010 3:00:00 PM
Topics: Guest Author, Health & Wellness
Preparing Your Athletes For Rotational Exercises Part II - Advanced Rotary Movements
Posted by Boston Sports Medicine and Performance Group on Nov 21, 2010 3:00:00 PM
by Art Horne
In the previous article entitled, Are You Qualified? Preparing Your Athletes For Rotational Exercises, I discussed the need to qualify your athletes for rotary movement prior to employing a long and extensive list of rotational core exercises including medicine ball throws and high level chopping patterns.
Below are a few advanced movements we employ after our athletes have demonstrated mastery in the rotary movements outlined previously. It should be noted that some athletes, especially the taller athletes, might not ever get to some of these movements and strength coaches and athletic trainers must resist the urge to progress these athletes along with the rest of the group until they have clearly shown mastery at the previous level. Remember, although the tall guys enjoy a clear advantage around the rim, performing simple plank holds and/or other strength movements just takes a little bit more effort – including even some of the most elementary rotary movements.

A Note on the Latissiumus Dorsi as a Lumbar Stabilizer
In a previous interview with Low Back Expert, Dr. Stu McGill, he mentions the importance of engaging the lats during exercises to help stiffen the core and provide a stable and strong base to work from. This point should be emphasized and facilitated when teaching the following exercises and also reinforced with those athletes having trouble “locking” their rib cage to their pelvis. To do so, simply stroke the lats from the shoulder down and into the thoracolumbar fascia to help facilitate this massive lumbar stabilizer. (Note: this is a great technique also when teaching athletes to pull from the floor/blocks and during squatting to help prevent shearing forces at the lumbar spine)
Stir The Pot with 12 o’clock Reach
"Stir the Pot" has become a staple in our program, but eventually our stronger guards master this movement and some additional challenge needs to be given to them to keep them both interested and adapting to increased stress. Once your athlete has mastered the basic exercise, which means a stable lumbar spine with no movement from rib cage to pelvis the following challenges can be made.
1. Reduce the width of their base of support by bringing their feet closer together.
2. Add an additional reach forward at the 12 o’clock position. Yes, this is actually an advanced “anti-extension” exercise, but a simple addition to a great exercise that gives you an additional bang for your buck.
3. Note: if your athlete is having trouble executing the beginner “stir the pot” instead of yelling at them over and over to hold their core tight, offer some simple tactile feedback by “raking” or “stroking” the lats on both sides to encourage this massive lumbar stabilizer to engage. This simple facilitation maneuver will give your athlete the needed cueing they lack to lock their spine in place.
Palloff Press with Lateral Walk
As I mentioned in the previous article this exercise progression should begin on the floor in a tall kneeling position and then eventually make its way up to standing. Because we have limited Keiser machines in our facility we rarely incorporate this particular advanced movement into our team programming but proves to be an excellent exercise when working in smaller groups or one on one.
Have the athlete press the resistance away from their sternum and hold this position. From there, incorporate a lateral walk without losing a stable torso.
- Remember: the lumbar spine was made to resist rotary motion, not to produce it.
Post – Pull and Press
This is a simple chop/lift variation that we include with our post players that challenges them to transfer outside forces through a stable spine. Because the position and action “smells like basketball” compliance and effort is always high with this exercise.
- Position your athlete on a 45 degree angle with their back towards the Keiser machine. In a deep post or athletic position first pull the cable stick across your body while maintaining a stable base and spine. This position should smell a lot like a deep post position in which your athlete must sit and take up space while asking for the ball with hands in front.

who ever said basketball isn’t a contact sport never played in the post
- Finish by pressing cable stick forward. Return and repeat.
- Emphasize transferring external load and resisting external rotational forces in a strong athletic position.
Front to Side Bridge
Although plank positions in and of themselves are not rotary movements, transitioning from one to the other certainly employs a great amount of rotary resistance. We start this exercise progression as I would image most coaches would, with simple plank holds. We then transition this simple exercise into a 5x5 second front-side planks. The athlete will hold the side plank position for 5 seconds and then transfer to the front plank – easy right? Actually, it’s not. The key here is to not allow the athlete to disassociate their hips/pelvis from their spine. Transitioning from the side to front plank is certainly the easier of the two but requires a ton of oblique involvement to keep the top shoulder and top hip moving in unison. From there, a static 5 second hold is performed from which the athlete transitions back. The final progression, as shown in the video, is a continuous front-side plank position without holds at either position. This is extremely challenging. Rarely will your tallest athletes be able to complete this task on the floor. Start these athletes by leaning to the wall to both learn and master this movement.
** Remember - help your athletes achieve success by facilitating their lats with a few simple strokes and/or offering a small bit of assistance at either the shoulder or hips until they learn how to lock their rib cage and pelvis together.
Modification for the taller athlete
Medicine Ball Rotational Throws
Besides the traditional medicine ball throws that you have seen and used in your own programming, two that can be used to emphasize locking the rib cage to the pelvis as well as establishing a solid base and post position are the Split Stance Side Toss (used mostly with the guards) and the Over Head Pivot throw (used mostly with the post players).
a)Split Stance Side Toss
- Hold the medicine ball on outside hip in a split stance position
- pivot on inside foot while quickly rotating outside hip (locked into the rib cage) and medicine ball around to face the wall
- toss the medicine ball at the wall as hips becomes parallel with wall. Emphasize “locking” the rib cage and pelvis together during the throw and establishing a strong finish position while catching the ball returning from the wall.
b)OH Pivot Series
- Hold medicine ball above head while standing perpendicular to wall.
- Pivot on inside foot while “locking” rib cage and pelvis together so that shoulders and hip move in unison.
** in both of the above medicine ball activities an athlete with poor technique will lead with the hips or shoulders and not “couple” them together. Both end positions should be strong and seated emphasizing a strong athletic post position.
** although almost all healthy athletes will be able to complete these exercises with terrible technique and without pain, an emphasis must be made as with all medicine ball activities to produce power through the hips and resist motion in the lumbar spine. By allowing the rib cage and pelvis to become grossly separated repeatedly will increase the chance of aberrant motion throughout the lumbar spine and thus subsequent pain and injury to follow. Post players that are not able to resist an external force (ie – Shaq, but then again who can right?) separating their upper and lower body during a fight for a deep post position or rebounding position will often find themselves at a huge disadvantage.

To quote Dr. Stu McGill, “Athletes utilizing explosive rotational exercises in search of world class performance will always end up chewing up their backs prior to reaching the point of world class performance in which they were in search of.”
Keiser with MB dynamic lift pattern
As shown in the previous article, the lift pattern can become a dynamic exercise and one that clearly replicates an athlete working his way to the rim from the low block. Since many schools do not have the use of a Keiser unit or enough units to make this exercise practical in a large group setting, we have incorporated the Verti-max units and have shown this exercise here using the Verti-max while holding a Core-ball for additional external resistance. The goal of the exercise again is to resist rotary forces about the lumbar spine while producing this motion through the hips and “locking” the rib cage and pelvis together.
Closing Thoughts:
As with all exercises, mastery takes time. Resist the urge to progress an athlete to the next level of difficulty prior to mastering the basics. This may even mean taking the taller athletes off the floor and starting them on a table or wall. If you are unsure whether your athlete is prepared for a rotary activity simply have them perform the prone shoulder touch again or continue to incorporate this activity into your daily warm-up to help groove this pattern.
Topics: Art Horne, Health & Wellness
Functional Manual Reaction Of The Foot And Ankle by Gary Gray
Posted by Boston Sports Medicine and Performance Group on Nov 13, 2010 9:15:00 AM
Topics: Guest Author, Health & Wellness
Basketball And Knee Pain - Solving The Patellofemoral Mystery by Mike Reinhold
Posted by Boston Sports Medicine and Performance Group on Nov 13, 2010 9:06:00 AM
Topics: Guest Author, Health & Wellness
Pre-Season Training: It All Starts With The Feet by Alan Stein
Posted by Boston Sports Medicine and Performance Group on Nov 7, 2010 5:00:00 PM
by Alan Stein
www.StrongerTeam.com
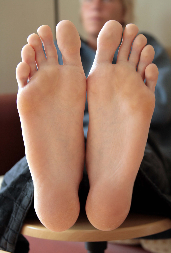
A basketball player’s feet are important. Let me rephrase that. A basketball player’s feet are extremely important. There are approximately 26 bones and 20 muscles in the feet. That fact alone should shed some light on their significance.
Basketball is (supposed to be) played standing upright on two feet. Therefore, every movement a player makes on the court is initiated through their feet. Every shot, every rebound, and every pass. Everything starts with the feet. With that said, can you guess what the most common injury is for basketball players at every level?
The ankle.
Strong and mobile ankles and feet will lessen the occurrence of injury, decrease the time lost if an injury does occur, and will improve performance on the court.
As obvious as these statements sound, most players and coaches put very littler priority on training the feet properly. The goal of this article is to change that.
Before I go further, let me make it crystal clear that this is not a research project or case study. My stance on training the feet and my opposition to ankle braces (and tape) is purely my opinion. I am in no way trying to refute the advice of a qualified athletic trainer or podiatrist or any legit study that has been conducted. However, my opinion is based on 10+ years of hands on experience in the field, thousands of hours of observations, a firm understanding of the human body and efficient movement, and numerous conversations with colleagues.
Basketball shoes are designed to be rigid (with stiff soles) to create as much stability as possible. To further increase stability, many players also wear ankle braces or get their ankles taped. Here lies the problem. By creating so much stability, they drastically limit mobility. Severely limiting mobility will weaken the muscles of the ankles and feet. What happens to a person’s forearm muscle when their arm has been immobilized in a cast from a broken wrist? It atrophies (weakens). So do the muscles of the feet when they are confined to rigid shoes and ankle braces for long periods of time. Many youth basketball players wear high top shoes and ankle braces 20+ hours per week!
I am not opposed to wearing basketball shoes when you are playing. The stability and support is a necessity. But you don’t need to wear them when you are training. And ankle braces? Tape? With the exception of a player who suffered a previous ankle injury, or someone taking a direct recommendation from a qualified medical professional… ankle braces (and tape) are absolutely unnecessary when playing and when training.
Still not convinced? When you get a chance, flip on ESPN Classic and watch any NBA game from the 1970’s. In addition to shorts that look like boxer briefs, every single player wore low top Adidas sneakers. No braces. No tape. And guess what? No injuries!
What did players wear before Adidas? Chuck Taylors! Thin canvas with a flat rubber sole. Talk about no ankle support! Despite the archaic footwear, there was actually a lower rate of ankle and foot injuries in the 60’s and 70’s than there is today. You know why? Players back then had strong, mobile ankles and feet.
Ankle braces weaken ankles and limit mobility (not to mention natural movement). Given how important the feet and ankles are, why would you do something that makes them weaker and less mobile?
Every time you run or jump, you do what is called triple extension. That is extension at the ankles, knees, and hips. If any one of those joints is not working properly (weak or tight), it limits the function of the other two. So weak, tight ankles limit a player’s ability to run and jump to their potential. Having weak, tight ankles will also cause the body to compensate in a variety of ways during movement… which can lead to knee and back issues. Remember, everything starts with the feet.
The same thing happens when you land from a jump or during each step when you run. The impact is supposed to be dissipated through your ankles, knees, and hips. Well, if your ankles are immobile and can’t move through a normal range of motion… that force and that impact is now directed to the next closest link in the chain… the knee! Weak, immobile ankles cause additional stress on the knees when landing and running.
So how do you strengthen your ankles and feet? By setting them free and taking off your shoes!
When you work out in your bare feet (or with socks) you can feel all of the intrinsic muscles of your toes, feet, and ankles. At first, this will feel liberating (and probably awkward) because you rarely get to feel these muscles when wearing basketball shoes and ankle braces.
NOTE: I am only suggesting barefoot training for players with healthy feet and no pre-existing conditions (unless cleared by a doctor). Players with excessively high arches, previous stress fractures, or ankle sprains should avoid barefoot training (or at least make severe modifications) to reduce the chance of injury.
How much is the right amount of barefoot training? Once a player has been acclimated to some rudimentary barefoot exercises, they should do as many things barefoot as they can in the confines of a safe, controlled training environment. For most players, 5-15 minutes per workout is a good rule of thumb.
If a player has been wearing ankle braces regularly for an extended period of time, they need to gradually wean themselves off of them. They should not go from wearing them all the time to not at all. Their ankles and feet aren’t ready for that. They need to begin a progressive, structured ankle and foot strengthening program, while at the same time slowly decreasing their dependence on the braces.
What should they do in their bare feet? Many of the same things they do with shoes on! Squats, lunges, dynamic flexibility movements, and low level hops are all great to do shoeless. Pick a few exercises each workout and rotate them. Begin with the most basic exercises and have the player progress as they become acclimated and their feet become stronger. Make sure you perform barefoot exercises on an appropriate surface (cautious of impact, slipping, etc.).
One of your goal’s this pre-season needs to be to improve foot and ankle strength, mobility, and proprioception (the body’s perception of movement and special awareness). If you do that you will lay the foundation for a championship season!
Topics: Health & Wellness, Alan Stein
A Review Of CNS Fatigue by Ryan Donahue
Posted by Boston Sports Medicine and Performance Group on Nov 7, 2010 4:51:00 PM

INTRODUCTION
Central Nervous System (CNS) fatigue is a topic so unexplored by the scientists of today that we still do not know the specific mechanism that causes it [1]. CNS fatigue, also referred to as neuromuscular fatigue, is a subjective state in which one feels tired or exhausted and in which the capacity for normal work or activity is reduced [17]. Muscle fatigue, the decline in voluntary force during sustained maximal efforts, is caused by both central and peripheral mechanisms [17]. It is widely known that much of the fatigue arises from processes occurring within the muscle such as disturbances in the excitation-contraction coupling, depletion of muscle glycogen and accumulation of metabolites [9]. Hence, It is believed that fatigue onsets at some point during the chain of events between the CNS and the stimulation of the muscle fiber [17]. There has been much speculation on whether central nervous system fatigue is a disease, such as chronic fatigue syndrome, or is it caused by a lack of energy and build up of waste product.
Distinguishing between peripheral and central fatigue, peripheral fatigue refers to events occurring within the motor unit [26]. Central fatigue involves events occurring in the brain and spinal cord [26].
Fatigue occurs at the neuromuscular junction when an action potential fails to cross from the motor neuron to the muscle fiber [17]. The neuromuscular junction, or motor endplate, is the interface between the end of unmyelinated and myelinated motor neurons and a muscle fiber [17]. Its main function is to transmit the nerve impulse and to initiate muscle action [17].
The purpose of this paper is to examine whether or not central nervous system fatigue can be delayed during exercise; as well as the potential causes for CNS fatigue, ultimately leading to its definition. We will accomplish this by first examining the excitation contraction – coupling process to revisit the basic process of motor unit stimulation. Following, we will move on to observe several studies going in depth on the effects of nutritional supplementations. The focal point of nutritional supplementations will be on Branched-Chain Amino Acids, Carbohydrate, and Caffeine.
Neurotransmitters will be the next focal point, in which the functions of Acetylcholine at the motor endplate will be examined closely. Along with acetylcholine, serotonin and its mood regulating qualities will be examined closely. Furthering the discussion of serotonin we will analyze several studies involving the 5-HT/Dopamine ratio which has shown profound effects on CNS fatigue during exercise [11]. Along with neurotransmitters, neuromodulators are also attributable to CNS fatigue. The most significant neuromodulators, Cytokines and Ammonia will be the ones examined.
This will lead us to the discussion of the possibility that central nervous system fatigue could be caused by a disease. Chronic Fatigue syndrome is a disorder associated with persistent physical and mental fatigue [11]. Lastly, an examination of the Central Governor Model [26] will give insight to the approach of CNS fatigue as a sensation or emotion, not a peripheral mechanism.
THE EXCITATION-CONTRACTION COUPLING PROCESS
In order to understand central nervous system fatigue one must take a step back and understand of how a muscle fiber twitch is stimulated. This is explained in the excitation-coupling process [9]. The excitation and contraction process that occurs at the neuromuscular junction leading to the ultimate goal of a muscle fiber twitch is a long and complicated process [9]. Essentially it begins with the stimulation of a motor neuron and the generation of an action potential that travels down the axon causing the release of Ca++ in the process [9]. The resultant influx of Ca++ into the nerve terminal leads to the exocytosis of vesicles containing Acetylcholine (Ach) [9]. The Ach then crosses the synapse, binding to receptors on the endplate region of the sarcolemma and generating an endplate potential causing an influx of Na+ [9]. This increase in Na+ results in a depolarization of the endplate [9]. The action potential generated then travels down the sarcolemma by way of the t-tubular network [9]. The voltage sensors bound to the t-tubule membrane are then stimulated and undergo a conformational change as a result of the action potential [9]. This leads to the opening of the Ca++ channels in the sarcoplasmic reticulum, causing an efflux of Ca++ [9]. With the present increase in cycstolic Ca++ concentration increase, Ca++ binds to Tropin C, causing a conformational change of tropomyosin [9]. The active site of actin is then exposed allowing the actin-myosin cross-bridge formation to occur and a muscle fiber twitch is stimulated [9].
It is believed that at some point during this excitation and contraction process a mechanism causes the onset of fatigue. Where and when is still unknown but several scientists believe that nutritional supplementation can delay the onset of CNS fatigue [2,3,4,5,10,12,13,14,20,21,22,23,24,25,27].
EFFECT OF BRANCHED-CHAIN AMINO ACIDS
Branched-chain amino acids are one supplement that has been researched extensively in endurance runners [13]. Prolonged exercise increases the plasma-concentration ratio of free tryptophan/Branched-chain amino acids (BCAAs), as well as the uptake of tryptophan by the brain [4]. The supplementation and intake of BCAAs may reduce the uptake of tryptophan by the brain and 5-HT synthesis, hence delaying fatigue [4,22]. Hassmen et al. [13] reported that 30-km cross country runners supplied with a mixed BCAA and carbohydrate solution during the 30-km race exhibited an increase in cognitive performance measured via the use of the Stroop Colour-Word Test. The Colour-Word test involves assessing words with variations of different colors, color words and regular words [5,13]. This increase was compared to a placebo group who performed the same exercise and showed no differences in the beverage they consumed [13]. Therefore, BCAA supplementation had a noticeable effect on more complex tasks [13]. Blomstrand et al. [4] demonstrated similar results in terms of the placebo group v. experimental group, in a study consisting of seven male endurance-trained cyclists performing exhaustive exercise on a cycle ergometer. During 60 minute exercise at a given work rate the subjects’ ratings of perceived exertion when they were given BCAAs were 7% lower, and their ratings of mental fatigue were 15% lower than when they were given placebo [4].
CARBOHYDRATE SUPPLEMENTATION
Carbohydrate is the main energy source for athletic performance [17]. To fully understand the effect on mental fatigue, we must review its peripheral effects [17]. High levels of blood glucose and glycogen stores located in the muscles and liver before any endurance exercise will lengthen time to exhaustion while delaying the onset of peripheral fatigue [17]. Carbohydrates have been demonstrated to increase performance while consumed during the actual exercise [17]. Muscles constantly require glucose, the end product of carbohydrates, for contractions of the muscles to produce a force [17].
When there is a decrease of blood glucose and an insufficient amount of glycogen stores in the muscle and liver to produce more, the muscles must seek elsewhere for an energy substrate [17]. A decline in blood glucose, hypoglycemia, during prolonged exercise will decrease exercise time to exhaustion and impair work output, thus causing fatigue [17].
Understanding the affects of carbohydrates on exercise in general, it must be known that nutritional status can alter brain neurochemistry [8]. Carbohydrate consumption before and during exercise inflicts a decrease in 5-HT concentration through a decrease in free tryptophan and tryptophan to the brain [8]. The decrease in 5-HT concentration represents a delay in fatigue and will be discussed later in this article [11]. Davis et al. [8] reported that cyclists who cycled for 225 minutes at 68% of their VO2max that received a 6 or 12% carbohydrate drink delayed the onset of fatigue. The placebo group in this study who received a water beverage during exercise exhibited a decrease in glucose and insulin levels, as well as a seven-fold decrease in the plasma-concentration ratio of free tryptophan/Branched-chain amino acids [8,20,21,23].
CAFFEINE SUPPLEMENTATION
Caffeine is the most commonly consumed drug in the world, and athletes frequently use it as an ergogenic aid [12,24]. Caffeine improves concentration, reduces fatigue, and enhances alertness [24]. It is believed that caffeine enhances neuromuscular transmission and improves skeletal muscle contractility. However, acute caffeine ingestion does not seem to increase maximal voluntary contractions or maximal power output nor delay fatigue [27]. Using caffeine as a supplement can also be detrimental to those who become dependent on it. In this case withdrawal of caffeine can increase fatigue as well as irritability, headaches, and mood swings [27].
Kalmar et al. [14] found that caffeine may increase the descending drive from the motor cortex by blocking the inhibitory effects of adenosine, which then increased a subject’s ability to excite a motor unit pool. Adenosine is a nucleoside comprised of adenine and ribose that is the structural component of nucleic acids and the major molecular component AMP, ADP, ATP [17]. The excitation of the motor unit pool could increase synaptic input to the cell body of the alpha-motorneuron by increasing its excitability, bringing the motorneuron closer to threshold, and facilitating maximal activation [14]. An increase in activation of spinal or supraspinal mechanisms may represent an increase in motor unit recruitment or an increase in the discharge rates [14]. It was also stated that caffeine may exert its effect on the neuromuscular system peripherally, by altering excitation-contraction coupling [14]. However, more research is needed to ultimately determine the effects of caffeine on the central nervous system.
NEUROTRANSMITTER FUNCTION AND CNS FATIGUE
Acetylcholine (Ach) is the primary neurotransmitter involved in the autonomic nervous system, especially at the motor endplate [17]. In regards to the motor endplate, in low quantity acetylcholine elicits a muscular contraction and in large quantity acetylcholine can actually inhibit the muscular contractions resulting from the stimulation of the nerve [9]. Within the neuromuscular junction there are approximately 50 to 70 vesicles containing Ach per um2 of nerve terminal area with a diameter of 30 to 50 nm [9,28]. These vesicles are strategically placed within the neuromuscular junction so that the clusters of Ach can be directly across from their postsynaptic receptors [9].
During fatigue it is speculated that Ach is increased at the NMJ and therefore causes inhibition of the nerve stimulation at the NMJ [28]. Different modalities of exercise elicit different response of Ach at the NMJ. Training at high-intensity has resulted in a greater dispersion of Ach receptor and vesicle clusters within the overall nerve terminal and endplate areas, thus resulting in a decrease in stimulation and ultimately greater fatigability [28].
Wilson and Deschenes [28] also noted that endurance exercise increased the nerve terminal area and pre- and post- synaptic areas, where as resistance exercise increase the postsynaptic area. The pre-synaptic area is the nerve terminal containing the Ach vesicles lying close to but do not come in contact with the sarcolemma [17]. The postsynaptic area on the other hand is a component of the sarcolemma located adjacent to the synaptic cleft [17].
Increases in hypertrophy due to resistance training have also shown to increase Ach at the NMJ [28]. With hypertrophy, the increase in muscle size elicits an increase in the size of the NMJ which in turn will require a proportionate increase in Ach to elicit adequate stimulation of the greater muscle fiber, thus delaying fatigue [28].
Serotonin is another neurotransmitter playing a large role in the determination of CNS fatigability. In brief, serotonin plays a large role in the regulation of mood in the brain and is widely considered the main argument of CNS fatigue [18,19]. Serotonin has been linked to fatigue because of its well known effects on sleep, lethargy and drowsiness, and loss of motivation [18,19]. However, serotonin itself cannot be attributed to fatigue alone, it is more effective when associated with dopamine.
The serotonin/dopamine ratio or 5-HT/dopamine ratio can be directly associated to fatigue [11,22]. If 5-HT production is high and dopamine production is low, this causes an imbalance in the 5-HT/dopamine ratio, which in turn elicits reduced exercise performance [11]. Conversely, if 5-HT production is low and dopamine production is high then this imbalance should cause an increase in performance, thus delaying fatigue [11].
Decreased 5-HT production results in less 5-HT turnover in the brain and thus there would be a less subjective feeling of fatigue [11]. As a result the tryptophan/BCAA ratio should be balanced in this case [11]. Likewise, increased dopamine production would cause an increase in mood state, which would not result in fatigue but result in more motivation, concentration and enhanced performance [11].
NEUROMODULATORS AND CNS FATIGUE
Neuromodulators are released by neurons and immune cells to convey information to adjacent or distant neurons, either enhancing or inhibiting their activities [17]. The neuromodulators that are most influential CNS fatigue are Cytokines and Ammonia [15]. Increases in cytokine levels have been associated with reduced exercise tolerance associated with acute viral or bacterial infection [7]. Along with the findings of Davis et al. [7], Katafuchi et al. [15] found that cytokines play a large role in hypothalamo-pituitary and sympathetic activation, as well as immunosuppression. Ammonia on the other hand, has been observed to negatively affect the CNS function due to the accumulations of ammonia in the blood and brain during exercise [7]. However, further research is needed to clarify the actual effects of these two neuromodulators.
CHRONIC FATIGUE SYNDROME
Could the cause of central nervous system fatigue be a disease? This has been debated amongst scientists for years to date. Chronic fatigue syndrome (CFS) is a disorder associated with persistent, often debilitating, physical and mental fatigue that cane be aggravated by even modest degrees of physical activity [11,16,29]. CFS can onset suddenly or gradually. The majority of CFS cases onset suddenly, with the beginning of another disease, such as the flu or another illness [11,29]. Other sudden onsets of CFS can occur during a period of significant physical or emotional stress [11]. The gradual arrival of CFS begins with mild symptoms that slowly increase over time [11]. Usually these patients are negligent that anything is wrong for awhile and attribute symptoms to other illnesses or stress [29].
Some of the symptoms experienced by individuals with CFS along with fatigue include disturbances to the autonomic nervous system, psychological disturbances, sleep patterns, poor temperature control, hypersensitivity, cognitive problems, and pain [11,29].
Georgiades et al. [11] examined the acute exercise related responses of circulating amino acids that have influenced the central 5-hydroxytryptamine (5-HT; Serotoninergic) system and dopamine function relative to subjects with similar physical activity histories.
In using the cycle ergometer test, the subjects with CFS exhibited a higher rate of perceived exertion (RPE) than the subjects without, which could lead to the indication that CFS leads to altered perception of work output [11]. RPE is the individual’s perception of how hard they are working based on a scale ranging from 6-17 and very, very light to very, very hard [11]. The RPE exhibited by the CFS individuals most likely attributed to the lower peak VO2max rather than a true maximum [11].
In CFS patients, 5-HT levels have been deemed the most significant difference in subjects with the disease and those without [11]. The increase in brain 5-HT concentration can be linked to the lower RPE due to higher turnover rate of 5-HT in the brain [11]. The high rate of 5-HT turnover is linked to an imbalance of the plasma-concentration ratio of free tryptophan/Branched-chain amino acids [11,21,22]. Tryptophan is an essential amino acid and a precursor for serotonin [22]. The imbalance of the plasma-concentration ratio of free tryptophan/Branched-chain amino acids is most likely due to an increase in free tryptophan, hence the high turnover exhibited by 5-HT in the brain [11,22].
Along with the 5-HT system, the dopaminergic system has also been implicated in central fatigue during exercise [11]. Dopamine is a chemical naturally produced by the hypothalamus and is commonly referred to as a “reward” neurotransmitter [17]. If there are high levels of arousal, motivation, and physical performance, dopamine is usually present [17]. Tyrosine, an essential amino acid and precursor to dopamine, had very low levels in the CFS at all time points including rest, therefore a mechanism must be limiting its production [11].
Analyzing the findings on 5-HT and Dopamine with CFS patients, it can be determined that if 5-HT production is high and dopamine production is low, then the 5-HT/Dopamine ratio is unbalanced, which in turn elicits reduced exercise performance [11]. In addition, the free tryptophan/tyrosine ratio implicates fatigue due to high effort perception via the RPE (Borg) Scale [11].
The cause of CFS however cannot be entirely attributed to CNS factors. Other factors must be taken into consideration, such as the individual’s heterogeneous nature and the fact that this disease is a multistage disease [11]. At different stages in this disease different values of 5-HT and dopamine as well as their precursors must be examined carefully for they could have different implications [11,16,25].
These considerations can be accomplished by through assessment and treatment modalities. Some treatments suggest drug therapy intervention to reestablish the chemical levels in the brain but this has not been proven scientifically [11,25]. The best way to approach therapy in CFS is cognitive-behavioral therapy, which helps identify and exclude factors contributing and maintaining chronic fatigue [16].
CENTRAL GOVERNOR MODEL
One of the more recent propositions on CNS fatigue is the Central Governor Model (CGM). The CGM “proposes that exercise performance is regulated by the central nervous system specifically to ensure that catastrophic physiological failure does not occur during normal exercise [26].” In essence, the main focal point of this model is to stress that peripheral fatigue cannot be used as a primary and direct influence on performance, rather fatigue should be considered a sensation or emotion, not connected to a physical manifestation [26].
The CGM offers a unique perspective on the bodily response to the tasks such as the Wingate test. The Wingate test is a high intensity cycling test that measures anaerobic exercise capacity and is typically performed for 30 seconds [26]. Contrary to the popular belief that fatigue during the Wingate test is caused by an accumulation of Pi and ADP, the CGM states that fatigue is cause by a reduced rate of motor unit recruitment by the CNS [26].
Assessed through an Electromyographic (EMG) response from the rectus femoris, Weir et al. [26] reported that findings have actually been contradictory to the CGM. According to the CGM, the EMG amplitude should decline as the brain decreases motor unit recruitment to avoid rigor [26]. Analyzing the results from the EMG in the Wingate test, it suggested that the central neural drive remains unchanged during the test, so peripheral mechanisms must explain the power output reduction [26]. However, this is not consistent when examining events that require a pacing strategy.
Events requiring a pacing strategy such as the 100m dash and 400m dash offer results that directly contradict the findings in the Wingate test [26]. In examining high intensity, short duration exercise, the bodily decisions to adopt a pacing strategy is not contingent metabolic events because a metabolic steady state is not achieved so expeditiously [26]. Can a dramatic increase in pace during the last 5-10% of a race, such as a 400m dash, be attributed to peripheral mechanisms when fatigue is assumed to be at its highest? According to Weir et al. [26] it cannot be associated to peripheral mechanisms. Weir et al. [26] responded further by proposing that the CNS regulates motor unit recruitment so that ATP consumption and production are matched, preventing rigor. Therefore it is safe to predict that fatigue occurs faster where ATP demand is the greatest [26].
CONCLUSIONS
Taking into consideration the physiological factors, as well as the nutritional and neuromuscular adaptations in CNS fatigue we must ask ourselves again, is it possible to delay CNS fatigue during exercise?
It has been shown through few nutritional factors that fatigue may perhaps be delayed [2,3,4,5,10,12,13,14,20,21,22,23,24,25,27]. But there is still much to debate on how much of that is attributed to peripheral fatigue. Certainly the supplementation of carbohydrates will delay fatigue [8]. After all carbohydrates are the main energy sources for athletic performance [17]. Carbohydrate consumption before and during exercise was demonstrated to inflict a decrease in 5-HT concentration through a decrease in free tryptophan and tryptophan to the brain [8].
Caffeine could either delay fatigue or begin the onset of fatigue sooner than it has had in the past [12,14,24,27]. The variable in this is the individual. Whether the individual uses caffeine in the right and controlled manner in respect to their body composition will determine its overall effect on delaying CNS fatigue [24]. Caffeine after all is classified as an ergogenic aid by most and a waste by others [12]. It was shown through several studies that caffeine had no acute effects on maximal voluntary contractions or maximal power output nor delaying fatigue [27]. So perhaps the effect of caffeine can be seen as a “placebo effect,” in that by taking caffeine, individuals would function under the assumption that this ergogenic aid is giving them “new life” while exercising [24]. If the literature states that caffeine has no acute effects on maximal voluntary contractions and maximal power output, is it safe to assume that perhaps it does chronically? It may be for individuals dependent on the substance, but in all reality it most likely does not.
BCAAs on the other hand, I believe do have a significant effect on CNS fatigue, especially when combined with carbohydrates as exhibited in the study by Hassmen et al [13]. The use of the Stroops Colour-Word Test showed uncompromisable results that cognitive performanced by the five to seven fold [5,13]. Blomstrand et al. [5] reported that the supplementation and intake of BCAAs may reduce the uptake of tryptophan by the brain and 5-HT synthesis and was exhibited vividly cycling study. Given the subjects’ ratings of perceived exertion when they were given BCAAs was 7% lower and their ratings of mental fatigue was 15% lower than the placebo group, there is no doubt that BCAAs are effective in delaying CNS fatigue [5].
The correlation between BCAAs and 5-HT synthesis has implied that 5-HT could delay CNS fatigue [22]. Serotonin plays a large role in the regulation of mood in the brain and when coupled with dopamine in the 5-HT/dopamine ratio, there is reason to believe that it does indeed elicit an effect on CNS fatigue [11,22]. The imbalance of the 5-HT/dopamine ratio, favoring an increase in 5-HT synthesis and a decrease in dopamine secretion is the most practical way to approach the effect of the two neurotransmitters [11]. Due to their physiological defined characteristics; serotonin related to mood and dopamine as a “reward” hormone, it was assumed that their imbalance would lead to CNS fatigue, and possible a chronic case of fatigue [11].
The most influential neurotransmitter, Acetylcholine, I believe cannot be attributed to CNS fatigue other than its physiological factors. Deschenes et al. [9] demonstrated in low quantity, acetylcholine elicits a muscular contraction and in large quantity acetylcholine can actually inhibit the muscular contractions resulting from the stimulation of the nerve. Under only the previous conditions alone can Ach be attributed with fatigue because otherwise it does not appear to have any other affect [9,17]. With hypertrophy Ach increases in the number of Ach containing vesicles but that is only primarily due to the increase in size of the neuromuscular junction in order to keep pace with the hypertrophic demands of the body [9]. Hence it is still undetermined whether Ach plays more of a role in CNS fatigue and the possibility of Ach delaying CNS fatigue.
Revisiting the question posed earlier, is CNS fatigue the result of a disease or the build up of waste product? The conclusion must be that both are attributable to CNS fatigue albeit a build up of waste product is more in the peripheral area of fatigue. Chronic Fatigue Syndrome was examined extensively and proved to make valid statements in discussing the 5-HT/dopamine ratio [11]. Although other factors must be taken into consideration when attributing CNS fatigue to CFS, it is hard to overlook the fact that perhaps right now we could be at a different stage of CFS, just not exhibiting a majority of the symptoms [16]. Our values of 5-HT and dopamine as well as their precursors could be imbalanced [11,16]. The use of the RPE scale in CFS patients as opposed to non-CFS patients as reported by Georgiades et al. [11] proposes valid points about CFS patients’ interpretations of their work outputs, but this alone cannot be the determinant of whether CFS is the cause of CNS fatigue.
The Central Governor Model poses one of the most interesting perspectives on fatigue. The proposition states that fatigue is due to a sensation or emotion experienced by the brain and not by a peripheral mechanism [26]. Specifically, it proposes that the subconscious bran determines the metabolic cost that is required to perform a given task [26]. The task that is interpreted by the brain is regulated to the extent that if motor unit recruitment is to high, the brain will decrease recruitment in order to avoid a terminal metabolic crisis and catastrophe via production and retention of Pi and ADP [26].
After extensively researching and forming opinions about the possible factors causing CNS fatigue, it is more than apparent that much more experimentation is needed to fully grasp this concept. Much speculation has been proposed about neurotransmitters and neuromodulators but there is no “gold standard” to measure the effectiveness of each. The same applies as to whether CNS fatigue is caused by a disease or not. We simply are not at the technological point we need to be at in order to effectively determine fact from speculation.
The studies examined throughout this paper have contradicted each other to numerous degrees. The various theories and explanations surveyed through this study all posed valid points, however the degree to which they contradict unfortunately is enough to note that the true definition of CNS fatigue is not feasible at this point. Essentially what we accomplished through this paper was form a definition of what does not delay, cause, or is responsible for CNS fatigue. The true effects of the internal and external variables in relation to CNS fatigue require much further research and experimentation.
REFERENCES
Anish EJ. Exercise and its effects on the central nervous system. Current Sports Medicine Reports. 2005 February;4(1):18-23
Blomstrand E. Amino acids and central fatigue. Amino Acids. 2001;20(1):25-34.
Blomstrand E. A role for branched-chain amino acids in reducing central fatigue.
Journal of Nutrition. 2006 February;136(2):544S-547S.
Blomstrand E, Moller K, Secher NH, Nybo L. Effect of carbohydrate ingestion on brain exchange of amino acids during sustained exercise in human subjects. Acta Physiologica Scandinavica. 2005 November;185(3):203-9.
Blomstrand E, Hassmen P, Ek S, ekblom B, Newsholme EA. Influence of ingesting a solution of branched-chain amino acids on perceived exertion during exercise. Acta Physiologica Scandinavica. 1997 January;159(1):41-9.
Davis JM. Central and peripheral factors in fatigue. Journal of Sports Sciences. 1995 Summer; 13 Vol. No:S49-53.
Davis JM, Bailey SP. Possible mechanisms of central nervous system fatigue during exercise. Medicine and Science in Sport and Exercise. 1997 Jan;29(1):45-57.
Davis JM. Alderson NL, Welsh RS. Serotonin and central nervous system fatigue: nutritional considerations. American Journal of Clinical Nutrition. 2000 August; 72(2 Suppl): 573S-8S.
Deschenes, Micheal R., Carl M. Maresh and William J. Kraemer. 1994: The Neuromuscular Junction: Structure function, and its role in the Excitation of Muscle. The Journal of Strength and Conditioning Research: Vol. 8, No. 2, pp. 103-109.
Gandevia SC, Taylor JL. Supraspinal fatigue: the effects of caffeine on human muscle performance. Journal of Applied Physiology. 2006 June; 100(6): 1749-50.
Georgiades E, Beham WM, Kilduff LP, Hadjicharalambous M, Mackie EE, Wilson J, Ward SA, Pitsiladis YP. Chronic fatigue syndrome: new evidence for a central fatigue disorder. Clinical Sciences (London). 2003 August; 105(2): 213-8.
Graham TE. Caffeine and exercise: metabolism, endurance and performance. Sports Medicine. 2001;31(11):785-807
Hassmen P, Blomstrand E, Ekblom B, Newsholme EA. Branched-chain amino acid supplementation during 30-km competitive run: mood and cognitive performance. Nutrition. 1994 Sep-Oct;10(5):405-10.
Kalmar JM, Cafarelli E. Central fatigue and transcranial magnetic stimulation: effect of caffeine and the confound of peripheral transmission failure. Journal of Neuroscience Methods. 2004 September 30;138(1-2):15-26.
Katafuchi T, Kondo T, Take S, Yoshimura M. Brain cytokines and the 5-HT system during poly I:C induced fatigue. Annals of the New York Academy of Sciences. 2006 November; 1088: 230-7
Lieb K, Dammann G, Berger M, Bauer J. Chronic fatigue syndrome. Definition, diagnostic measures and therapeutic possibilities. Der Nervenarzt. 1996 September;67(9):711-20.
McArdle, William D., Frank I. Katch, Victor L. Katch. Exercise Physiology: Energy, Nutrition, and Human Performance 6th Edition. Baltimore, Maryland: Lippincott Williams & Wilkins, 2007.
Meeusen R. Exercise and the brain: insight in new therapeutic modalities. Annals of Transplantation: quarterly of the polish transplantation society. 2005;10(4):49-51.
Meeusen R, De Meirleir K. Exercise and brain neurotransmission. Sports Medicine. 1995 Sep;20(3):160-88.
Newsholme EA, Blomstrand E. Branched-chain amino acids and central fatigue.
Journal of Nutrition. 2006 January;136(1 Suppl):274S-6S.
Newsholme EA, Blomstrand E. The plasma level of some amino acids and physical and mental fatigue. Experientia. 1996 May 15; 52(5):413-5
Newsholme EA, Blomstrand E. Tryptophan, 5-hydroxytryptamine and a possible explanation for central fatigue. Advances in Experimental Medical Biology. 1995;384:315-20.
Newsholme EA, Blomstrand E, Ekblom B. Physical and mental fatigue: metabolic mechanisms and importance of plasma amino acids. British Medical Bulletin. 1992 Jul;48(3):477-95.
Paluska SA. Caffeine and exercise. Current Sports Medicine Reports. 2003 August;2(4):213-9.
Sharpe M, Chalder T, Palmer I, Wessely S. Chronic fatigue syndrome. A practical guide to assessment and management. General Hospital Psychiatry. 1997 May;19(3):185-99.
Weir JP, Beck TW, Cramer JT, Housh TJ. Is fatigue all in your head? A critical review of the central governor model. British Journal of Sports Medicine. 2006 Jul;40(7):573-86;
Williams JH. Caffeine, neuromuscular function and high-intensity exercise performance. The Journal of sports medicine and physical fitness. 1991 September;31(3):481-9.
Wilson MH, Deschenes MR. The neuromuscular junction: anatomical features and adaptations to various forms of increased, or decreased neuromuscular activity. The international journal of neuroscience. 2005 Jun;115(6):803-28
Wyler VB. The chronic fatigue syndrome – an update. Acta Neurologica Scandinavica Supplementum. 2007;187:7-14.
Ryan Donahue, CSCS, Is an Assistant Strength & Conditioning Coach at Northeastern University, Boston MA, where he is also currently working to complete a Doctorate in Physical Therapy. Ryan received his B.S. from the University of Connecticut where he also worked with many of the university’s athletic programs, including football. Ryan can be reached at ryan.a.donahue@gmail.com.
Topics: Guest Author, Health & Wellness
More Glutes Please: Part II by Art Horne
Posted by Boston Sports Medicine and Performance Group on Oct 30, 2010 11:32:00 PM
by Art Horne

It’s clear that good glute function and strength underpins good knee health – especially in the basketball athlete. However, despite the loads of research from the likes of Powers and Ireland supporting this concept, many athletes still continue to suffer despite our best efforts to strengthen the hip musculature and specifically the Gluteus Medius (GM).
Let’s take a closer look at what may be missing from your current GM training.
The Janda Approach
Janda identified two groups of muscles based on function within both the upper and lower body and classified them as either “tonic” or “phasic”. The tonic group of muscles consists of the “flexors”, while the “phasic” muscle group consists of the “extensors” and work eccentrically against gravity. Because of their position and function, Janda noted that the tonic muscles are prone to tightness and shortness while the phasic muscles are prone to weakness and inhibition.
With regards to knee pain, this concept is well regarded and accepted when dealing specifically with the iliopsoas and gluteus maximus among basketball strength coaches and athletic trainers. Not only is the iliopsoas short and tight in most basketball athletes, and the gluteus maximus inhibited, but it is also well accepted that this iliopsoas “tightness” causes a reflexive reciprocal inhibition and thus may be a contributing cause to the phasic nature of the gluteus maximus. In fact, one could spend an extraordinary amount of time “facilitating” the gluteus maximus with retraining or activation exercises, but until the iliopsoas’ tonic nature is reduced these exercises may very well be futile. This is similar to the light switch in your home office. You can flick your office light switch on and off all you want (activation), but unless there is electricity getting to that switch (reduced tone in the iliopsoas) those lights just aren’t coming on.
Flexor Withdrawal Reflex
Definition: a common reflex consisting of a widespread contraction of the physiologic flexor muscles and relaxation of physiologic extensor muscles; characterized by an abrupt withdrawal of the body part in a response to a painful stimuli.
I first learned about this reflex in school where I memorized it for the exam and soon forgot about it until this “phenomenon” was discussed again upon visiting Nico Berg (speaker at the 1st Annual Boston Hockey Summit) in Vancouver BC Canada during a summer learning trip. During my visit he so kindly pointed out to me that after injury, not just after touching a hot stove as we were all taught, that the body undergoes this flexion “contracture”. Take for example the common ankle sprain – extension of the ankle (dorsiflexion) is never the position that an athlete will choose to splint themselves in after injury. Plantar flexion is the preferred motion and thus a loss of Achilles length is the normal consequence of crutch walking after ankle sprain. Yes, gravity has a lot to do with the foot flopping down into this prolonged plantar flexed position, and of course the sheets on your bed further aggravates this problem as you lay helpless against the power of your cotton comforter and gravity, but neither of these can be associated with the flexion “contracture” found in both the knee and elbow after injury. When was the last time you heard an athlete having trouble getting their flexion back after knee surgery?
Let’s take a look how this flexion pattern may relate to knee pain, adductor tightness and ultimately glute med dysfunction.

In this case some would argue that the chicken came before the egg when it comes to PFPS (patellofemoral pain syndrome – or good ol’ fashion knee pain) and associated glute med weakness. For this argument, let’s just say that the knee pain, and hence the painful stimuli, happened first. As we mentioned before the body will undergo a “flexion” contracture or flexion type pattern. Normally, when discussing flexion at the knee the most common sagittal plane flexion-extension movement comes to mind, but for the sake of this argument let’s instead focus on the frontal plane “flexion” pattern.
“But Art, that’s called adduction!”
Call it what you want – but we would all agree that the knee and the surrounding musculature moves and shortens towards the body’s midline – (hip adduction, femur internal rotation and flexion – some actually call this combined motion pronation, but that’s for another day) - think fetal position.
Needless to say, the adductor group similar to your gastroc-soleus complex after an ankle sprain, hamstrings after a knee injury and biceps after elbow insult, become short - agreed?
Enter Sherrington’s law of reciprocal inhibition (Sherrington, 1907), which states that a hypertonic antagonist muscle may be reflexively inhibiting its agonist! Therefore, in the case of our glute med strengthening exercises, the presence of these tight and/or shortened adductors (antagonistic muscles), restoring normal muscle tone and/or muscle length must be addressed first before attempting to strengthen the weakened or inhibited gluteus medius (agonist muscles). (Page)
“Wait a second, I’ve heard this before.”
Yes, you probably have. In fact, Janda so famously described this trend as the Lower Crossed Syndrome. Unfortunately, so much attention has been given to the interplay between psoas tightness and gluteus max dysfunction that I think we’ve forgotten about max’s little brother medius.
Same challenges, same solutions.
Tightness and on one side of the joint with inhibition on the other.
Putting It All Together
My challenge is simply to take this concept (that you are already employing with the hip flexor and gluteus max) one step further and apply to the tonic Hip ADDuctors and the Gluteus Medius – two muscles that sit on opposite sides of the joint similar to the iliopsoas and gluteus maximus.
Taking the tone out of the Adductor Group
Prior to beginning any gluteus medius strengthening work, encourage your athletes to address the soft tissue restrictions within the adductor group with one or both of the below foam roller techniques and follow up with a kneeling hip adductor stretch.
Remember, frantically flicking the light switch on and off won’t get electricity to the light bulb unless power is running into your house first.
Encourage your athletes to address the entire adductor group from origin to insertion. For shorter athletes this is easy by having them "unload" their weight as needed and addressing on a treatment table. Taller athletes often need a taller table or some additional coaching.
For those athletes that need additional help, some light over-pressure from a coach or athletic trainer while taking their femur through their available internal and external range of motion is often helpful. Warning: Athletes with existing knee pain tend to be very tender over the adductor group as it crosses the knee - especially the first time. As this "tone" and discomfort becomes less, so does the athlete's anterior knee pain. In fact, it is my experience that you can predict which athletes have anterior knee pain and which leg their knee pain exists by the amount of tenderness athletes describe during this maneuver.
Follow up your foam rolling with some adductor stretches in an effort to sustain this new tissue quality and length.
References
Beckman SM, Buchanan TS. “Ankle inversion injury and hypermobility: Effect on hip and ankle muscle electromyography onset latency.” Arch Phys Med Rehabil. 1995; 76(12):1138-1143.
Biel A. Trail Guide to the Body. 3rd Ed. Boulder, CO: Books of Discovery; 2005.
Distefano LJ, et al. “Gluteal Muscle Activation During Common Therapeutic Exercises.” Journal of Orthopaedic & Sports Physical Therapy. 2009. Vol. 39. No. 7. 532-540.
Drake RL, Vogl W, Mitchell AWM. Gray’s Anatomy for Students. 1st Ed. Philadelphia, PA: Elsevier Churchill Livingstone; 2005.
Fredericson M, Cookingham CL, Chaudharis AM, Dowdell BC, Oestreicher N, Sahrmann SA. “Hip abductor weakness in distance runners with iliotibial band syndrome.” Clin J Sports Med. 2000; 10:169-175.
Friel K, McLean N, Myers C, Caceres. “Ipsilateral hip abductor weakness after inversion ankle sprain.” J Athl Train. 2006; 41(1):74-78.
Henriksen M, Aaboe J, Simonsen EB, Alkjaer T, Bliddal H. “Experimentally reduced hip abductor function during walking: Implications for knee joint loads.” J Biomech. Accepted March 11, 2009, not yet in print.
Ireland ML, Wilson JD, Ballantyne BT, Davis IM. “Hip Strength in females with and without patellofemoral pain.” J Orthop Sports Phys Ther. 2003. 33(11):671-6.
Janda V. 1987. “Muscles and motor control in low back pain: Assessment and management.” In Twomey LT(Ed.) Physical therapy of the low back. Churchill Livingstone: New York. Pg. 253-278.
Khaund R, Flynn SH. “Illiotibial Band Syndrome: A Common Source of Knee Pain.” Am Fam Physician. 2005; 71(8):1545-1550.
Nadler SF, Malanga GA, Feinberg JH, Prybicien M, Stitik TP, DePrince M. “Relationship between hip muscle imbalance and occurrence of low back pain in collegiate athletes: a prospective study.” Am J Phys Med Rehabil. 2001; 80(8):572-577.
Nakagawa TH, Muniz TB, Marche Baldon RM, Maciel CD, Menezes Reiff RD, Serrao FV. “The effect of additional strengthening of hip abductor and lateral rotator muscles in patellofemoral pain syndrome: a randomized controlled pilot study.” Clin Rehabil. 2008; 22: 1051-1060.
Nelson-Wong E, Gregory DE, Winter DA, Callaghan JP. “Gluteus medius muscle activation patterns as a predictor of low back pain during standing.” Clin Biomech. 2008; 23:545-553.
Page, P. Frank C. The Janda Approach to Chronic Musculoskeletal Pain.
Presswood L, Cronin J, Keogh JWL, Whatman C. “Gluteus Medius: Applied Anatomy, Dysfunction, Assessment, and Progressive Strengthening.” Strength and Conditioning Journal. 2008; 30(5): 41-53.
Sahrmann. Diagnosis and Treatment of Movement Impairment Syndromes.
Sherrington CS. 1907. “On reciprocal innervations of antagonistic muscles.” Proc R Soc Lond [Biol] 79B:337.
Shimokochi Y, Shultz SJ. “Mechanisms of noncontact anterior cruciate ligament injury.” J Athl Train. 2008; 43(4):396-408.
Souza RB, Draper CE, Fredericson M. Powers CM. “Femur Rotation and Patellofemoral Joint Kinematics: A Weight-Bearing Magnetic Resonance Imaging Analysis.” Journal of Orthopedic & Sports Physical Therapy. 2010. Vol 40:5. 277-285.
Starky C, Ryan J. Evaluation of Orthopedic and Athletic Injuries. 2nd Ed. Philadelphia, PA: F. A. Davis Company; 2002.
Umphred DA, Byl N, Lazaro RT, Roller M. 2001. “Interventions for neurological disabilities.” In Neurological Rehabilitation (Umphred DA, ed) 4th ed. Mosby: St. Louis. 56-134.
Wilson E. “Core Stability: Assessment and Functional Anatomy of the Hip Abductors.” Strength Cond J. 2005; 27(2):21-23.
Topics: Art Horne, Health & Wellness
More Glutes Please - Part One by Art Horne
Posted by Boston Sports Medicine and Performance Group on Oct 23, 2010 10:53:00 AM
Are you hammering your athlete's glutes or just hammering your head against the wall?
Many athletic trainers and strength coaches will prescribe glute med work in their programs whether it be for rehabilitation, activation exercises before training or simply as part of an athlete's maintenance work - yet many of the problems for which we prescribe this work continues to show its ugly head during the basketball season.
Lets take a closer look at the work we are doing for the gluteus medius and what we might be missing in our athlete's program.
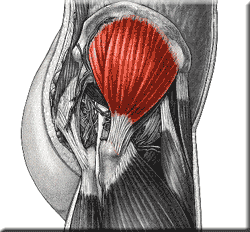
Origin: External surface of ilium between anterior and posterior gluteal lines.
Insertion: Lateral surface of the greater trochanter.
Innervation: Superior Gluteal Nerve (L4, L5, S1)
Function
All fibers abducts femur at the hip joint. Anterior fibers flex and medially rotate the hip. Posterior fibers extend and laterally rotate the hip. Most importantly, it holds the pelvis secure over the stance leg and prevents pelvic drop on the opposite swing side during walking.
Assessment
Palpation
With your patient/athlete side-lying, isolate the shape of the gluteus medius by placing the webbing of one hand along the iliac crest (from PSIS to nearly the ASIS) while the hand locates the greater trochanter. Your hands will form the pie-shaped outline of the gluteus medius. Palpate in this area from just below the iliac crest to the greater trochanter for the dense fibers of the gluteus medius. Ask your patient/athlete to abduct his/her hip slightly and you should feel the gluteus medius contract. (See attached diagrams.)
Hip Abduction Strength Test
• The patient is side lying with test leg on top.
• The therapist stands behind the patient and stabilizes with one hand at the hip, proximal to the greater trochanter.
• The other hand applies resistance across the lateral surface of the knee.
• Patient abducts hip against downward resistance
• If the patient is unable to perform the test side lying, place them in a supine position and feel for a gluteus medius contraction as they attempt to abduct their legs along the table.
• Note: During side lying hip abduction testing, Wilson (2005) points out that athletes “with weak hip abductors will attempt to compensate by recruiting their tensor fascia lata (flexing their hip), their external rotators (lateral pelvic rotation), or their quadratus lumborum (“hiking” their hip).”
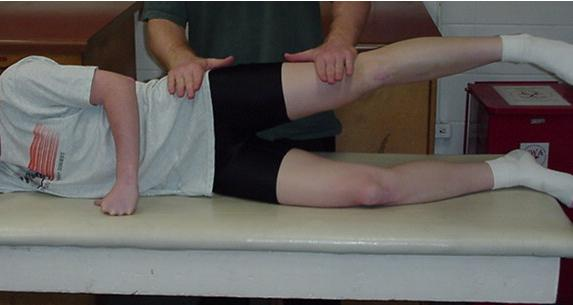
Trendelenburg’s Test for Gluteus Medius Weakness (Starkey, p293)
• Patient Position: Standing with weight evenly distributed between both feet.
• Lower patient’s shorts to the point that the iliac crests or PSIS is visible.
• Examiner Position: Standing, sitting, or kneeling behind patient.
• Procedure: The patient lifts the unaffected leg, standing on the affected leg.
• Positive Test: Pelvis lowers on the non-weight-bearing side.
• Implications: Insufficiency of the gluteus medius to support the torso in an erect position, indicating weakness in the muscle of decreased innervation.
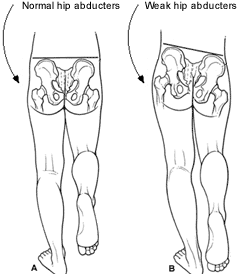
Implications of Gluteus Medius (GM) dysfunction
Why we do what we do
Presswood et al (2008) state that “a weak or dysfunctional GM is linked to numerous injuries of the lower extremities and abnormalities in the gait cycle.” (p 41) The authors cite past research that implicates a weak/dysfunctional gluteus medius in Trendelenburg gait (see above), lower back pain, Iliotibial band syndrome, patellofemoral pain syndrome, ACL tears and other knee injuries, and ankle injuries. (p 42-43)
Trendelenburg Gait
During walking if a person’s GM, on either side, is weak the hip of the leg currently in the swing phase of walking will drop tilting the pelvis laterally. (See Trendelenburg Test above for more information) Presswood et al state that this will reduce gait efficiency and may lead to decreased running speed, and possibly lower back pain since that pelvis is not stabilized properly during activity. (p 42)
(Weak and inefficient Glute Med. on the basketball court = ENERGY LEAK during Cross Over Dribble. Want to move in the front plane more efficiently? Train the Frontal Plane.)

Lower Back Pain
Research published by Nelson-Wong et al (2007) showed that, “Muscle activation patterns at the hip may be a useful addition for screening individuals to identify those at risk for developing low back pain during standing.” (p 545) Twenty three subjects, 12 men and 11 women, were made to stand in a constrained position for 2 hours while their hip muscle activity was monitored. 65% of those studied developed low back pain during the test, and 76% of those subjects had reduced GM activation. Additionally, Nadler et al (2001) showed that hip muscle imbalance, specifically with GM weakness, was strongly associated with low back pain in female athletes.
Iliotibial (IT) Band Syndrome
Khaund and Flynn (2005) state that IT band syndrome “is caused by excessive friction of the distal iliotibial band as it slides over the lateral femoral epicondyle during repetitive flexion and extension of the knee resulting in friction and potential irritation.” (p 1545) Key clinical recommendations in this article are that hip abductor weakness can contribute to IT band syndrome, and that strength training emphasis needs to be placed on the gluteus medius. (p 1546) The authors go on to cite research by Fredericson et al (2000) that concluded that, “Long distance runners with ITBS have weaker hip abduction strength in the affected leg compared with their unaffected leg and unaffected long-distance runners. Additionally, symptom improvement with a successful return to the preinjury training program parallels improvement in hip abductor strength.” (p 169)
Patellofemoral Pain Syndrome (PFPS)
Presswood et al (2008) cite research that defines PFPS as “an overuse injury characterized by anterior knee pain, often aggravated with stairclimbing, squatting, or sitting for prolonged periods of time.” (p 42) The authors go on to state that “inhibition or dysfunction of the GM may contribute to decreased hip control, allowing greater femoral adduction and/or internal rotation. This produces a larger valgus vector at the knee, increasing the laterally directed forces acting on the patella and contributing to the patella tracking laterally.” (p 42)
Nakagawa et al (2008) set out to study the effect of strengthening PSPS diagnosed patients’ quadriceps along with the hip abductors and lateral rotators (intervention) vs. just strengthening the quadriceps (control). Only the patients who were in the group strengthening the hip abductors and rotators improved their perceived pain symptoms. The intervention group not only had a reduction in pain, they also had increased knee extension torque and GM EMG activity. The control group’s only change was an increase in knee torque.
ACL Injuries

Presswood et al (2008) states that excessive “knee valgus or rotation of the femur during landing is a potential mechanism for ACL injury.” (p 43) The authors go on to say that athletes with a high level of GM control and strength are better prepared to counter these movements. In addition, female athletes have a 6-8 times greater chance of ACL injury, possibly due to increased “knee valgus and/or hip rotation [relative to] male athletes.” (p 43)
Shimokochi et al (2008) searched for literature regarding noncontact ACL injuries between 1950 and 2007, to ascertain possible mechanisms of injury. After finding and analyzing 40 articles meeting their criteria, the authors’ main conclusion was that ACL “injuries often happen when an individual attempts to decelerate the body from a jump or forward running while the knee is in shallow flexion angle. At the time of injury, combined motions such as knee valgus and knee internal-external rotation are often noted.” (p 406) They also noted that the ACL is “loaded with anterior tibial shear forces. Unopposed quadriceps muscle forces produce anterior shear forces, possibly damaging the ACL, especially near full extension.” (p 406) These conclusions support the need for not only proper GM function to avoid ACL injuries, but also the need for proper hamstring strength and function to counteract overt quadriceps dominance, along with excessive knee valgus and rotation.
Ankle Injuries
Friel et al (2006) tested a group of 23 people, ages 18 to 52 years old, with a history of at least 2 ankle sprains to the same side with no injury to the other side, and no traumatic lower extremity injury with 3 months. The study found that the strength of the hip abductors on the previously injured side was significantly reduced compared to the uninvolved side. Based on past research the authors stated that “After lower limb ligamentous injuries, dynamic postural control of the lumbopelvic hip complex decreases.” (p 76) Coupled with past data and results of the current study, the authors concluded that if a person’s hip abductors are weak they will be unable to counteract normal lateral sway during gait, which can potentially lead to ankle injury.
Additionally, Beckman et al (1995) studied the reflex latency response of hip and ankle muscles during ankle inversion. The authors concluded that subjects with ankle hyper mobility had decreased latency (the gluteus medius fired prematurely) of hip activation after ankle inversion. The researchers hypothesized that this was a protective measure coordinated by the body’s motor neurons that compensate for the hyper mobile ankle, and they concluded that clinicians must address altered hip muscle recruitment patterns in patients with ankle sprains.
Suggestions for Improving Function and Strengthening the Gluteus Medius
Presswood et al, in the authors’ review of past gluteus medius literature, state that generally patients are “prescribed open-chain or single-leg stance exercises to initially strengthen the GM in a side-lying or weight-bearing position. Closed chain exercises are introduced during the later stages of rehabilitation, once basic strength has been developed.” (p 44-45)
In reference to sets, reps, and frequency, the authors go on to cite a position statement by the American Council of Sports Medicine states that “at least 2 training sessions a week that involve 2 to3 sets of between 6 to 15 repetitions per set will lead to considerable increases in muscular strength and endurance.” (p 50) However, every patient is different, so the authors go on to reference the book, Techniques in Musculoskeletal Rehabilitation (McGraw-Hill Profession, 2001), and state that “for rehabilitation, strengthening exercises should be performed on a daily basis initially, with the number of repetitions and sets controlled by the patients’ level of pain, swelling, and response to exercise. As healing progresses, the muscle can be exercised every second day so the frequency becomes 3 to 4 times per week. Thus the exact loading parameters would appear to be dependent on the person’s injury and may vary between individuals.” (p 50)
With this in mind, the main goal of a GM strengthening program is to progressively overload the muscle so that it continues to develop muscular strength, control, and endurance. Review the article “Gluteus Medius: Applied Anatomy, Dysfunction, Assessment, and Progressive Strengthening” by Presswood et al as a starting place for more details.
Click here to view Common Gluteus Medius Strength Exercises.
Click below to view Uncommon Gluteus Medius Strength Exercises that you wish you were doing.
Summary
So what does this all mean and how does this apply to Basketball perforamance and health?
1. A strong and efficient GM is important in maintaining a healthy basketball athlete - Low back pain, knee pain and ankle problems (smells a lot like what keeps basketball athletes from playing the most doesn't it?) are all affected by GM dysfunction and weakness. Filling this gap in their training and maintenance program is the first step in keeping them on the floor.
2. Basketball = Knee Pain (or at least it used to). At one time basketball athletes were condemned to live out their careers with chronic knee pain because, "thats just part of the sport." With the work of Powers, Ireland and others, knee pain can be addressed by first attacking the hip (Charlie Weingroff presented on the importance of the Vertical Tibia and Knee Pain at this past year's Basketball Specific Conference ) and specifically addressing the GM. So turn off your ultrasound machines and get back to some good old fashion hip strengthening exercises.
3. Performance: a strong GM along with a trained and efficient Quadratus Lumborum/Obliques (lateral line) makes change of direction specifically in the frontal plane much more explosive and with less energy leakage enabling your athletes to move left to right at the speed of light.
Next week: Why all your glute med work still isn't working - The missing piece
Topics: Art Horne, Health & Wellness
Roll Out by Brijesh Patel
Posted by Boston Sports Medicine and Performance Group on Oct 3, 2010 4:25:00 PM
Topics: Health & Wellness, Brijesh Patel
